Postmenopausal bleeding confuses many of us, women and providers alike. While postmenopausal bleeding does not usually mean something is wrong, you should never ignore it. But before we get into causes and treatment, let’s start with some definitions, so we are all on the same page.
What exactly is postmenopausal bleeding?
Postmenopausal bleeding is ANY bleeding that happens after you go through menopause. Menopause is defined as going a full year without having any bleeding or periods. A couple of brown blood spots on your underwear ten years after your last period? Postmenopausal bleeding. Weekly spotting for the past two months, two years out from menopause? Postmenopausal bleeding. A gush of blood after sexual intercourse five years after your last period? Postmenopausal bleeding.

What is postmenopausal bleeding if you don’t know if you are postmenopausal yet? Perimenopause confuses many of us because it can be hard to know precisely when you have crossed the finish line of the perimenopause marathon. And it can be a marathon – perimenopause lasts anywhere from a few months to 12 years before your last period. It is a time of fluctuating menopausal symptoms that drives so many of us literally crazy. It is normal for periods to be irregular during perimenopause, with some women going months without any bleeding, followed by heavy bleeding for weeks afterward. According to the North American Menopause Society (NAMS), approximately 90 percent of women experience four to eight years of menstrual cycle changes before going through natural menopause.
Some women mistakenly ignore irregular bleeding after menopause because it may have happened regularly during perimenopause. However, even abnormal or irregular bleeding during perimenopause should be evaluated, according to the American College of Obstetricians and Gynecologists (ACOG) and NAMS. But what needs to be evaluated and how?
The connection between postmenopausal bleeding and endometrial cancer
Endometrial cancer is the big elephant in the room that all women’s health providers worry about for perimenopausal and postmenopausal women. Endometrial cancer starts in the lining of your uterus (womb), called the endometrium. It occurs most often after menopause in women in their 60s. Endometrial cancer is the most common cancer affecting the female reproductive organs, more common than ovarian cancer or cervical cancer. So what is the connection between postmenopausal bleeding and endometrial cancer?
Endometrial cancer occurs when endometrial cells (building blocks of your womb lining) start to grow and make copies of themselves too quickly. Perimenopausal and postmenopausal fluctuations in the balance of estrogen and progesterone cause changes in the endometrium. A disease or condition that increases the amount of estrogen but not the level of progesterone can increase your risk of endometrial cancer. When not balanced with progesterone, these higher estrogen levels can cause excessive growth and thickening of your endometrial cells. Women with larger bodies are at greater risk for endometrial cancer because fat tissue can also produce estrogen, resulting in higher estrogen levels acting on their endometrial lining.
The uterine lining may thicken in certain places, forming a tissue mass called a tumor. As your lining thickens, it becomes unstable, meaning it can fall off or be shed, coming out through your cervix and vagina just like it did with your periods. The key here is that any bleeding after menopause, no matter how irregular, light, or seemingly inconsequential, could be an early sign of endometrial cancer. Ninety percent (9 out of every 10 women) with endometrial cancer reported bleeding before their cancer diagnosis. Just remember that the reverse is not true. Not every woman with postmenopausal bleeding has endometrial cancer.
Endometrial cancer can be treated and cured, if it is caught early
Healthcare providers can detect endometrial cancer in its earlier stages because it frequently causes abnormal vaginal bleeding early on. When discovered early, removing the uterus surgically (hysterectomy) often cures endometrial cancer. With an early diagnosis, a woman has a 95 percent chance of surviving cancer for at least five years. That is why paying attention to irregular bleeding during perimenopause and menopause could save your life.
How to NOT ignore postmenopausal bleeding
So, how can you pay closer to your perimenopausal or post-menopausal bleeding? Keeping a record or calendar of your bleeding episodes through your menopausal transition helps you and your healthcare provider look for any patterns or red flags. Tracking your period is empowering and may be the most important proactive step you can take.
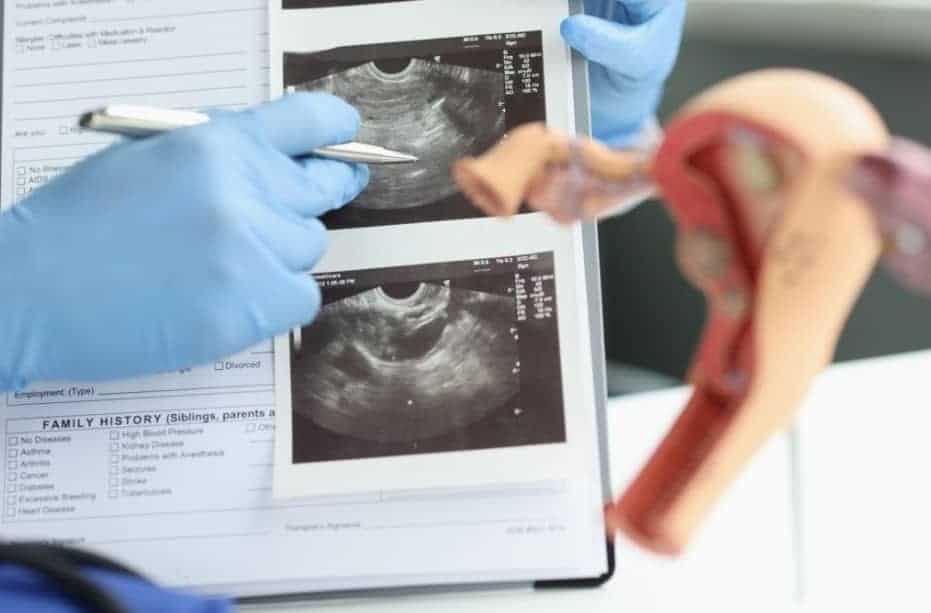
The next step is usually to have a transvaginal ultrasound. This non-invasive procedure can be done at your healthcare provider’s office or an ultrasound clinic. The ultrasonographer uses a wand-like transducer to measure the thickness of the endometrial lining. They also look to see if there are any abnormal tissue growths.
Combined with some tests to measure hormone levels, your provider can decide whether to take a closer look. If your endometrial lining measures thicker than four millimeters on the ultrasound, they will do an endometrial biopsy. This simple, in-office procedure is similar to a Pap smear and samples your endometrial lining. A laboratory can then examine your endometrial cells to look for pre-cancerous changes.
So while you might be tempted to ignore intermittent bleeding, especially if it seems to go away, you should not. Simply put, women who experience post-menopausal bleeding should have it evaluated as soon as possible. Earlier detection of abnormal cells or cancer could save your life. So while your postmenopausal bleeding most likely is not something to worry about, please don’t take the chance that it could be endometrial cancer.
If you have questions about midlife changes in your menstrual cycle or have had postmenopausal bleeding, please contact your healthcare provider or a North American Menopause (NAMS)-certified provider to get the answers your health depends upon.
Leave a Reply